01



Helmed by board-certified orthopedic and spine surgeon, Dr. Joshua S. Rovner, our center specializes in diagnosing the source of your neck and back pain and achieving relief through minimally-invasive surgery, so that you can get back on your feet and enjoy your active lifestyle with ease once again. Many consider that Dr. Rovner delivers some of the best spine surgery NJ has to offer, so you are in good hands with Dr. Joshua Rovner.





A global leader in robotic spine surgery
Dr. Joshua Rovner
As one of the best spine surgeons in NJ, Dr. Joshua S. Rovner provides surgical treatment of pain related to the neck and entire back. Dr. Rovner is one of the few providers of spine surgery in New Jersey that specializes in both minimally invasive spine surgery and robotic spinal surgery. These procedures are safer and more precise alternatives to traditional surgery and are shaping the future of spinal and orthopaedic medicine. By helping individuals leverage more progressive means of minimally-invasive spine surgery, Dr. Rovner helps his patients undergo a smoother surgery with faster recovery times.
A patient-centered and personalized approach enables Dr. Rovner and his New Jersey spine surgery team to diagnose and treat problems related to deformity, trauma, and degenerative conditions. From traditional procedures like lumbar spinal fusion, sports medicine and disc replacement surgery to more advanced and minimally-invasive techniques like robotic spine surgery, Dr. Rovner is one of the most comprehensive and experienced providers of spine surgery available.


Dr. Rovner Named a Top Doctor by Castle Connolly




With Dr. Rovner, the Emphasis is on You
At Progressive Spine and Orthopaedics, Dr. Rovner’s years of experience and professional skills are completely focused on you. Expect a thoughtful, individualized approach that truly takes you into account as an individual. Dr. Rovner dedicates his time to understand your concerns, correctly assessing your pain and your needs, and designing a personalized surgical plan that achieves your goals.
Patients choose Dr. Rovner instead of the impersonal experience at big hospitals because Dr. Rovner performs every surgery himself. Major hospitals are often teaching hospitals where patients are operated on by hospital residents, medical students, or fellows who lack experience. With Dr. Rovner, patients are operated on by an experienced, highly skilled, board-certified surgeon. Dr. Rovner is known for his patient care and results. His surgical skill is among the very best in the state.
Dr. Rovner begins with a detailed consultation to discuss your pain and your medical history. As he creates your custom surgical plan, he is dedicated to ensuring your surgical journey is precise and perfect from start to finish–designed specifically for you. Your experience, from preparing for surgery until you’ve fully healed, includes complete access to YOUR surgical team by email or phone at any time, 24 hours a day, seven days a week.

Dr. Fergie-Ross Montero-Cruz
Dr. Fergie-Ross Montero-Cruz
Dr. Montero-Cruz specializes in non-surgical treatments for musculoskeletal conditions, discomfort, and pain of the shoulder, elbow, hip, and knee. Her education and training are the foundation of her treatment protocols and the exceptional levels of relief she achieves for her patients.
More about Dr. Montero-CruzDr. David Porter
Dr. David Porter
Dr. Porter is a board-certified Orthopedic Surgeon that specializes in sports medicine issues in New Jersey such as knee and shoulder pain. His main goal is to minimize each patient's pain and help them regain normal physical function.
More about Dr. PorterDr. William Long
Dr. William Long
Dr. William Long is among New Jersey’s most accomplished spinal surgeons and is committed to treating a range of spinal conditions with non-surgical methods whenever possible. Dr. Long employs the most advanced techniques, including robotic surgery for superior results and a faster recovery time.
More about Dr. LongDr. Steven A.Bernstein
Dr. Steven A.Bernstein
Dr. Bernstein is Board Certified by the American Board of Foot and Ankle Surgeons and a highly trained and experienced Foot and Ankle Surgeon in Fort Lee and Secaucus NJ.
More about Dr. BernsteinSpine Conditions
Before we can treat your pain, we need to understand your condition. By locating the underlying cause of your symptoms first, we avoid unnecessary treatments, save time and money, and deliver the relief you need as quickly as possible. With years of experience diagnosing the full range of spinal disorders and diseases – both common and uncommon – few specialists are more qualified than Dr. Rovner. Providing patients with some of the best spine surgery NJ has to offer, Dr. Rovner will help educate you on your condition, and address your pain.



Spinal Conditions 01 Diagnosis 02
At Progressive Spine & Orthopaedics, our team of acclaimed spinal surgeons and pain relief specialists deliver a wide scope of non-invasive and surgical and non-surgical treatments for spinal conditions, including treating back pain, neck pain, spinal fractures, tumors, kyphosis, rheumatoid arthritis, sciatic nerve pain, herniated discs, scoliosis in adolescents, scoliosis in adults, spondylitis, stenosis, myelopathy, sacroiliac joint syndrome, spondylolisthesis, spondyloses, and spinal conditions affecting children. Our approach is to employ the least invasive, most effective treatments possible in every case.
The back and spine are some of the most complex systems in the body. Diagnosing spine or back pain requires a thorough examination and testing with the most advanced technology. Dr. Rovner and his team of certified medical professionals can accurately diagnose your condition prior to crafting a treatment plan to restore motion, reduce chronic pain, or treat and resolve a spinal injury or condition. Your treatment will be performed by a spinal surgeon in New Jersey who focuses on delivering the least invasive treatments, and who is at the forefront in the field of advanced spine and back treatments.
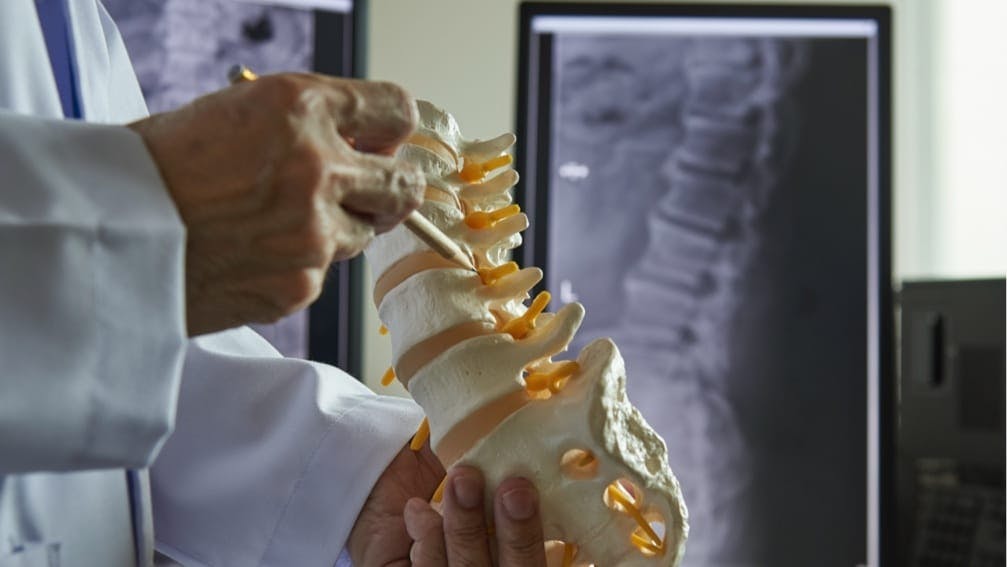
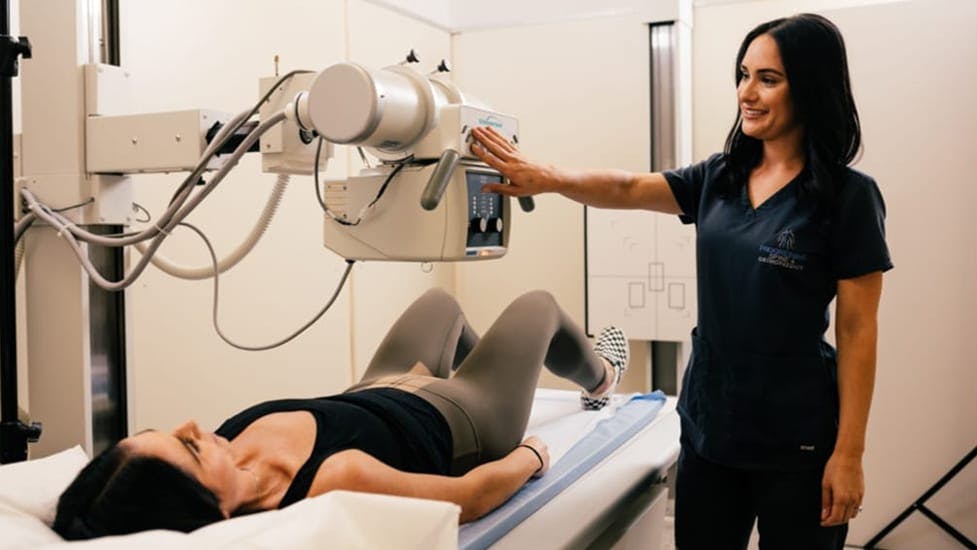




Groundbreaking treatments for spinal conditions
Spinal Surgeries
If you have exhausted all of your non-invasive treatment options and are ready for a more permanent solution to neck and back pain, Progressive Spine & Orthopaedics is one of the safest and most advanced surgical destinations in New Jersey. With a concentrated focus on minimally-invasive and robotic procedures, we leverage the latest surgical technology, instrumentation, and equipment available to resolve your chronic pain once and for all.




Leading New Jersey spinal surgeon
Dr. Rovner is a certified spine and orthopedic surgeon in Edison, NJ. Certified by the American Board of Orthopedic Surgeons and licensed to practice in the states of New York and New Jersey, spine surgeon Dr. Rovner takes a personal approach to his practice, putting the concerns of his patients at the forefront of his practice. This comes with the territory of being one of the top spine specialists NJ can offer the public.




Mazor Robotics System Robotic Spine Surgery
Our robotic procedures are performed with 3D surgical blueprints and one of the industry’s best robotic guidance systems – the Mazor Robotics System. Combined, these technologies provide a comprehensive plan for the procedure and direct Dr. Rovner’s instruments, ensuring unprecedented precision and increasing the likelihood of a successful surgical outcome.
One of the latest advances in spine treatment, robotic surgery gives our spine surgeon the ability to perform the necessary treatment with the highest level of accuracy. Known to reduce the risk of complications, boost accuracy, and reduce recovery time, robot-assisted surgery has proven to be far superior in results.
Advances in surgery have led to the development of robotic spine surgery. At Progressive Spine & Orthopaedics in New Jersey, our surgical team is dedicated to delivering the least invasive surgeries. If your spinal condition will not respond to a non-surgical treatment, we can perform robotic spine surgery, which is less invasive and has a faster recovery time. The procedure involves a specialized robotic system in which the surgery is performed with tiny surgical tools that respond to the precise motions of our spinal surgeon who is guided with real-time video. Our system, the Mazor Robotics System is the most advanced robotic system available, with the highest level of accuracy.



Follow Us on Instagram
@progressivespine
Our Partner Health Services
Discover comprehensive care with our affiliated brands, Progressive Wellness and NJ Vein Specialists, dedicated to enhancing your health journey