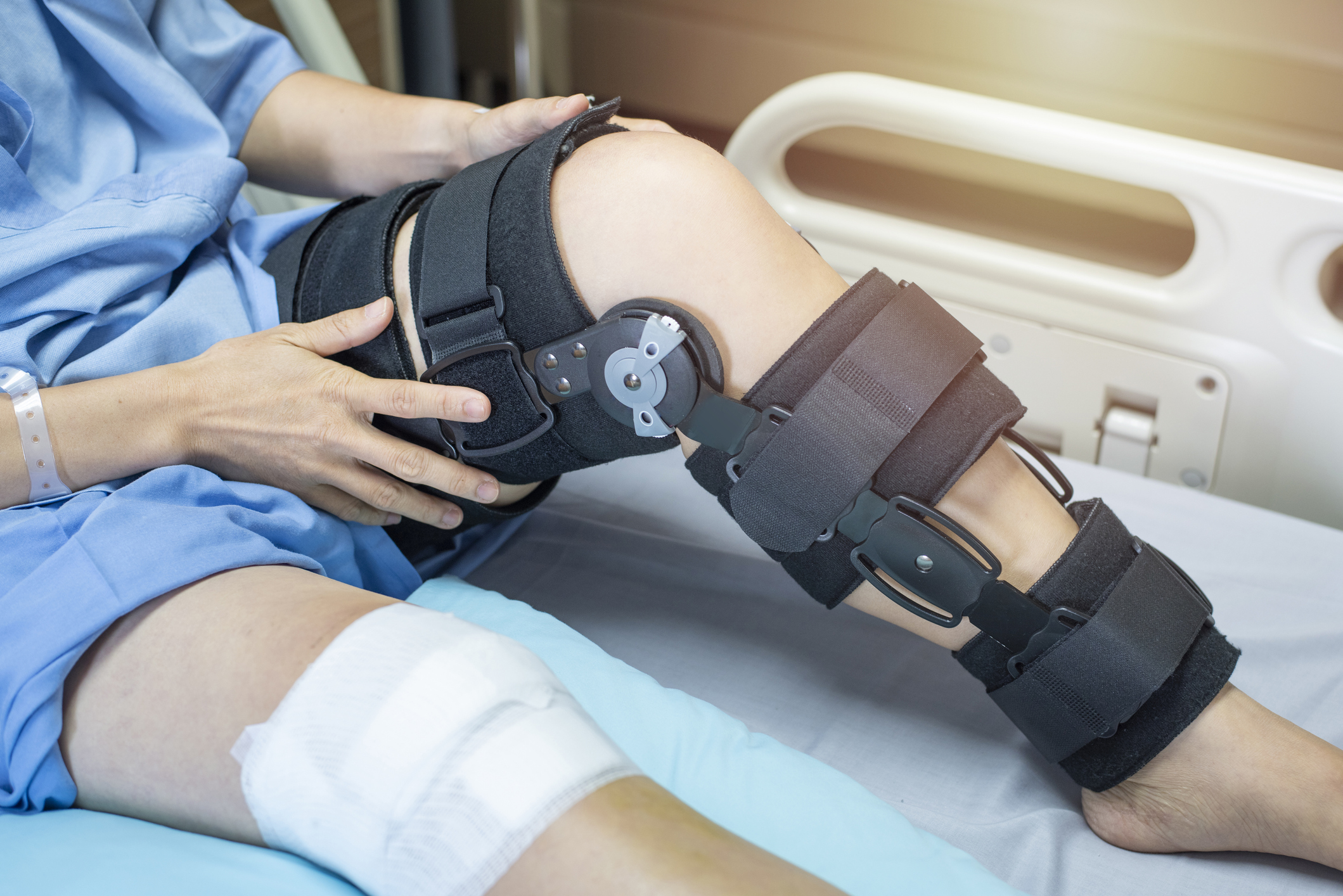
Dr. Rovner - Spine and Orthopedic Surgeon
Dr. Joshua S. Rovner, M.D., is a distinguished spine and orthopedic surgeon renowned for his expertise in minimally invasive surgical techniques. With a patient-centered and progressive approach, he has earned a reputation as a top spine specialist in New Jersey, providing unpara...
View More